|
It starts the moment you meet the patient. The neuro exam can be conducted quickly and is easy to integrate into your daily assessment. One reason may be that, unlike CT scans and other diagnostic tools, its results come in shades of gray, not black and white. Although it’s still an integral assessment component for critically ill patients, many bedside nurses overlook or underuse it. Subtle changes in findings may indicate the need for further testing.īefore the advent of computed tomography (CT) in the 1970s, the neurologic examination was the main tool used to monitor a patient’s neurologic condition. But once you become proficient in performing this exam, you’ll be able to detect early significant changes in a patient’s condition-in some cases, even before these show up on more advanced diagnostic tests. 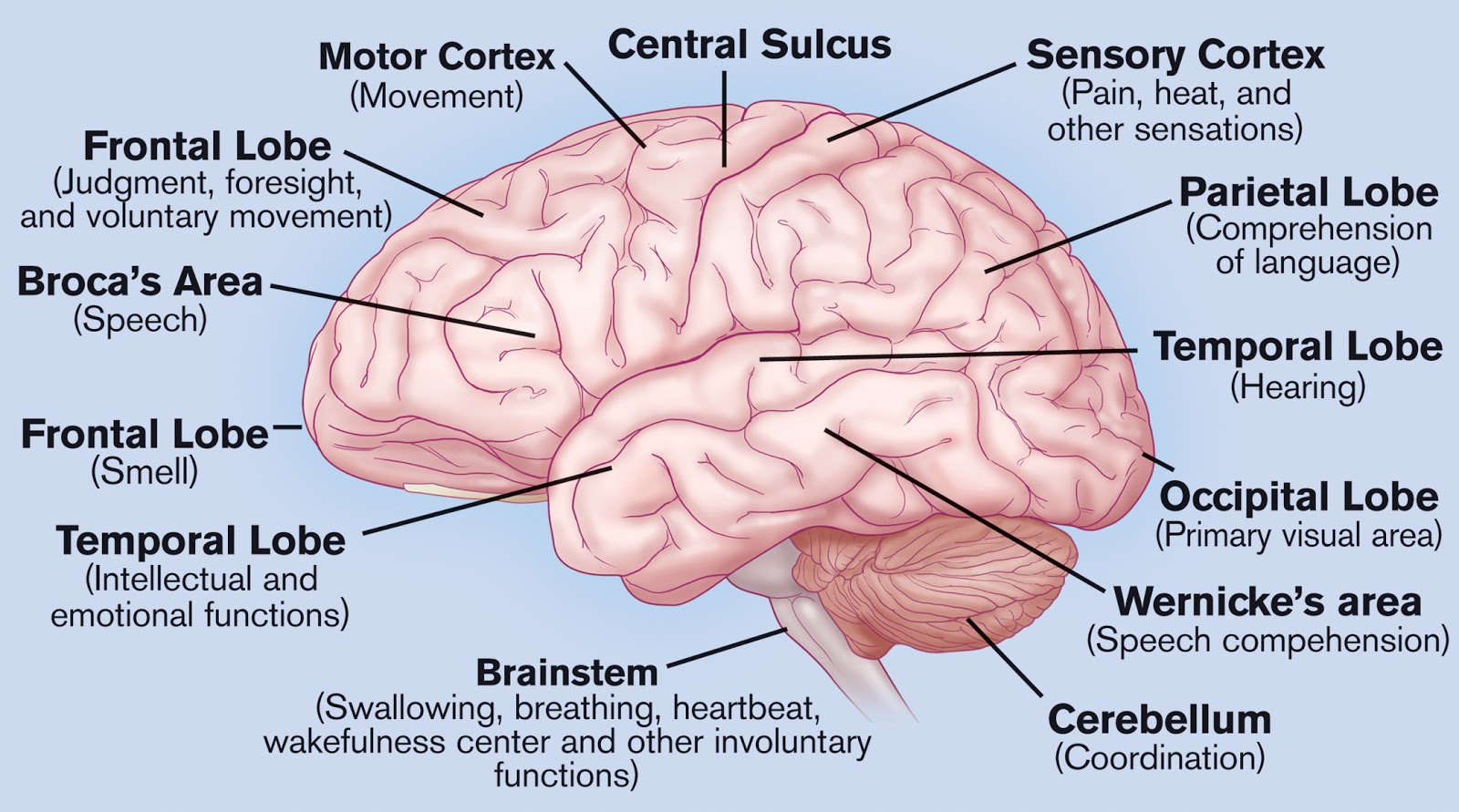
bmj.Assessing the neurologic status of unconscious or comatose patients can be a challenge because they can’t cooperate actively with your examination. Vegetative state: Term should be changed. Assessment scales for disorders of consciousness: Evidence-based recommendations for clinical practice and research. Maternal persistent vegetative state with successful fetal outcome. tbi/factsheets/vegetative-and-minimally-conscious-states-after-severe-tbi Vegetative and minimally conscious states after severe TBI. Unresponsive wakefulness syndrome: A new name for the vegetative state or apallic syndrome. Management of maternal vegetative state during pregnancy. nhs.uk/conditions/disorders-of-consciousness/ Persistent vegetative state and minimally conscious state. You can learn more about how we ensure our content is accurate and current by reading our editorial policy. Healthline has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. Those who do regain consciousness after an extended period may be left with severe disabilities due to brain damage. Recovery can still happen, but it’s highly unlikely. due to TBI and has lasted longer than 12 months.caused by nontraumatic brain injury and has lasted longer than 6 months.Recovery may be more difficult for people who experienced illness or nontraumatic brain injury. Some may be left with chronic disabilities. When an unaware and unresponsive neurological state lasts more than 4 weeks, it’s called a persistent vegetative state (PVS).Īmong people with TBI who remain in an unaware and unresponsive neurological state for a month, about 50 percent regain consciousness. There’s no way to accurately predict who will recover. Some will go on to lose all brain function. Some will gradually regain consciousness. People in an unaware and unresponsive state can transition to a minimally conscious state. What’s the outlook for individuals in this state? In some cases, the person may be transitioned to a nursing home or other long-term care facility. Treatment will begin in an acute care hospital setting. adding flowers, favorite perfumes, or other scents to the room.talking to them about things they’re familiar with. 
Various specialists may involve family members in trying to stimulate the senses and prompting a response by: management of bowel and bladder functions.physical therapy to gently exercise the joints.changing positions on a regular basis to avoid pressure sores.In addition, doctors will take steps to prevent potential complications, such as: The person will be carefully monitored for changes or signs of improvement. Rather, the focus is supportive care so the brain can heal. 
The person is conscious and fully aware but fully paralyzed and unable to speak. Damage to the brain and brain stem are categorically irreversible. The person alternates between awareness and lack of awareness. This unaware and unresponsive state differs from these similar conditions:
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
